Dr. Knoll on the Before, During, and After of Joint Replacement
- Comment
Toree: Hi, I’m Toree McGee, and this is The Rapid Recovery Report™, sponsored by ROMTech, the modern technology of rehabilitation. So, we’re going to be doing this series biweekly, I think, on Thursdays at 4:00pm Pacific and 7:00pm Eastern, where we talk to different guests. So, we’re going to have surgeons, and patients, and insiders here at ROMTech, physical therapists, just basically all kinds of people that are in the health industry to talk about wellness, health, and touch on ROMTech’s PortableConnect.
So, if you are new here, this little beauty is the PortableConnect. Isn’t she cute? It is a high-tech recovery device that is geared at getting patients moving faster. It’s got passive modes in it, and most importantly, all of the data that is happening while you are on this device at home is being sent to your surgeon, so that they can kind of keep tabs on you, and know what you’re doing at home.
So, if you want to learn a little bit more about us, you can visit us right there, at www.romtech.com, or follow our social media handles that are in the description below.
Joint Replacement Specialist Dr. Peter Knoll

But let’s talk about our guest that we’ve got here today. So, we’ve got Dr. Peter Knoll. He’s a joint replacement specialist at Tristate Orthopedic Surgeons in Evansville, Indiana. After graduating summa cum laude from the University of Notre Dame, he attended medical school at Case Western Reserve University, and then completed his residency in orthopedic surgery at Wright State University.
He continued his training with a fellowship in adult reconstruction at the University of Virginia, which allowed him a full immersion in all aspects of joint replacement and arthritis management.
Dr. Knoll’s practice includes the full spectrum of hip and knee replacements, including complex revisions and direct interior hips, as well as fracture, trauma care, and general orthopedics.
So, hi Dr. Knoll. Thank you for taking the time to hang out with us today.
Dr. Knoll: Hi Toree. My pleasure. Love to talk to you.
Toree: Perfect. So, this is something that I just feel like I have to know. We ask all of our surgeons this to start. So, what inspired you to make a career out of orthopedic medicine.
Dr. Knoll: So, it’s a good question. I always like medicine, and always felt that that was kind of an avenue I was going to go, but kind of if I didn’t do medicine, I feel like I’d be in some sort of physical science or something with physics and things like that. So, for me, orthopedics, and even specifically joint replacement really melds those two together, because you get the humanistic side and the patient care side of medicine, but also with the physics, with the science and biomechanics that I also enjoy. So, it really works as a nice combination, and really fits me well.
Preparing for Better Recovery Before Surgery
Toree: Good. Well, it sounds a lot more complicated than anything that I could do, so I’m glad that you went and did it instead of me. So, when we spoke with you a little bit before the show, you had shared with us the importance of what a patient does prior to surgery, and then also during recovery, and then following a complete recovery after an arthroplasty. So, we’re curious to learn, and share with our audience what does prehab mean.
Dr. Knoll: So, it’s a great question. Prehab is really, to me, kind of where it all starts. So, I use the analogy that if you decide you want to go run a marathon, generally you don’t just wake up on a Saturday morning, and go run a marathon, right? That’s probably not going to end really well for you. You’re going to start your training, right? You want to build your body up, and get ready for it. And the same is true for a surgery like a knee replacement.
So, for me, prehab is really a critical part, because intuitively, well, the stronger you are when you walk in that day of surgery, that’s much better position you are starting your recovery coming out. So, prehab, it’s a balance of being able to work on the range of motion, the strength. Understanding that, well, if you’re talking about surgeries because that knee doesn’t feel very good, so it’s hard to do, but there’s kind of specific exercises that can be done that are done in a gentle way, but you can get that strengthening and you can get that range of motion. We’re just going to set you up for success, and put you step ahead of where you were before the prehab, even before the surgery starts. So, it’s just all that, kind of the more you can do ahead of time to be ready for the surgery, well, the better your recovery is going to go.
Toree: Yeah. So, how long do you usually suggest prehab, and what are you asking your patients to do during that time?
Dr. Knoll: So, how long ahead of time? Usually, about the time we start talking about the surgery, that’s when I say, “Hey, start it.” The sooner you start training, the better. So, at least several weeks beforehand to really kind of get the knee in that mode, and get ready for it.
Some patients, for one reason or another, ends up their surgery is going to be a little further out, and I say, “Hey, go ahead and start now,” right? The more time we have, the stronger you can get.
So, the activities that we’re doing there is generally very low-impact things. So, it’s working on straight-leg raises, where it’s just synergy of bringing that leg up straight, and then lifting it up off the bed or the chair. It’s surprising how much that will work your quads, just lifting your legs without weights on it up off the bed a few times in a row, and that can really help straighten it.
I tell people, a couple of times a day, if they’re watching TV, you pop the heel up on an ottoman or a coffee table, put a bag of frozen peas, some little bit of weight on that knee helps stretch it out and straighten it out.
So, it’s not that I’m getting them in the gym and doing all these crazy workouts you see on TV or anything. It’s really pretty simple stuff, but it goes a long way to get that knee ready, get it as loose and as ready as we can to undergo surgery and start the recovery.
Toree: So, should I be doing leg lifts under my desk while I’m working?
Dr. Knoll: I would recommend it, yeah. It’s the same way on the other side. People tell me, “Hey, when should I stop doing the therapy?” I say never. It’s just it evolves. You can change from those early postop exercises to doing more general strengthening and everything else. But yeah, whether or not you have a knee arthritis, I mean, doing exercises is a great thing.
Toree: Yeah, not going to hurt.
Dr. Knoll: Exactly.
Typical Joint Replacement Recovery
Toree: So, once a patient undergoes a joint replacement, what does a typical recovery look like? And how long can a patient like expect for a complete recovery?
Dr. Knoll: Yeah, so that’s a great question. It’s a little different for everybody. Some of that, to go back to the prehab, it depends where you are when you start, right? And so, the stronger you’re coming in, the better your recovery is going to go. But in general, I look at the recovery in phases.
So, that initial phase is really just kind of getting over the acuity of the surgery, trying to get that swelling under control, and getting back that motion, because as soon as you have surgery the knee wants to stiffen up, and you got to kind of work against that to get that motion and everything. That’s that critical first couple of weeks there.
So, those first couple of weeks, in my mind, you’re kind of really focusing on that motion. As I tell patients, I’m not trying to get you go on long walks outside. I want you to get that motion, get that swelling out of there. And then once we achieved that goal, which hopefully is within that first 10 days or two weeks or so, then we start adding a little more of that activity. You’re up and walking during those first two weeks. It’s just not long distances or things like that.
Over those next couple of weeks, that’s when you’re getting out of the house, you’re taking some walks, you’re getting a little more active with it. May or may not still take a cane with you just to have some support, but you’re feeling like yourself a little more.
Once you get past that phase, that’s in that four to six-week range, that kind of thing, that’s where you start really get a little more adventurous. You’re going on longer trips to the store. People start to get back to the driving range and hitting some balls, and things like that. And then it’s just progressive from there.
So, complete recovery does take a while, but even though the number seems a long time to say, hey, it’s a couple of months before you’re yourself again, it’s not that you’re on bedrest for six weeks leading up to it. You’re getting better each day, each week. It’s just before you really say, “Oh my gosh, I can go do everything I want to do,” it does take some timing in there.

Getting Back to Normal Life
Toree: Yeah. So, now, are there special rehab instructions that you generally share with most of your patients? And does it differ if it’s like they’re arthritic, and that’s why they’re going through surgery?
Dr. Knoll: So, a little bit. What I do, because a lot of people come in, and they say, “What should I be doing at this point, how far shall we be walking,” and things like that. And I don’t put a specific on it, because everyone comes in at a different level. I mean, I can in the same day, do a surgery of someone who wants to get back to going skiing and rock climbing, and someone else who is more sedentary, and their goal is to get to the mailbox and back. So, they’re going to be, all along the way, a different timepoints of what they’re doing.
So, my instructions kind of go back to what I said, it’s more in the phases. You kind of got to crawl before you can walk, walk before you run. So, that’s that get that motion. So, I say, when I see you back – I usually see my patients back in two weeks. My more important thing is not how long of a walk have you gone on. It’s let’s me see your motion. How is your control of your quads? Can you straighten that leg out? Can you get the motion there? Once we established that, well, then yeah, start increasing it.
But I often tell people, I say, “Well, as you get to that phase where you’re doing more activity, kind of look at what you did today.” And if at the end of the day, you say, “Okay, my knee is still doing okay,” well then, tomorrow, do a little bit more.
But I don’t tell them, okay, today, go walk a quarter mile, tomorrow do a half mile, because everybody is a little bit different, as far as when they get to those points. It’s just as long as you are, each day, doing a little more, getting a little stronger, and doing a little more with that knee.
Toree: Yeah. Now, what happens when your patients don’t do the prehab, or if they don’t follow the rehab protocols? And do you have a lot of that?
Dr. Knoll: Fortunately, I don’t have a lot of that. I think the big thing there is explaining. I think it’s when people understand why they’re doing it, it makes a big difference. If you just say, “Here’s a list of exercises, go do them,” that doesn’t have the same effect as if you explain, well, this is why we do it, and this is how it’s going to help you, and how, in the long run, it’s going to be better for you.
Fortunately, I got a pretty good patient population that they’re going through this, they take some ownership, and they want to get better, and so that makes a big difference.
But yeah, other times, when people fall behind, definitely, so that’s where I’ll see them periodically, kind of check on their progress. And sometimes, it takes a little encouragement, because the knee hurts afterwards. There’s no if and buts about it. It does. And sometimes we feel that pain, and say, “Oh gosh, well, I think I might be doing damage here, and I hold off,” and so there can be that reason. Oh, I’m not going to do my exercise, because I think it might hurt more. So, coaching people that actually moving it, using it is going to help ease that out. It’s going to help make it better when you get back on track. And often times, that’s enough to get people back on track.
Sometimes, if we get really far behind, there are options where we can go in, and I can do kind of a guided total manipulation, where we get people some sedation. It’s a medication that really going to push through to help them get their motion. Fortunately, that’s pretty rare that we have to do that, because with the protocols we have in place and kind of checking on things and the checkpoints we hit, we can usually prevent it before it gets to that point.
Toree: Good, because that sounds not enjoyable at all.
Dr. Knoll: Yeah, it’s less than ideal. It’s a lot easier to stay on track with a therapy, and reach the goals a normal way.
Toree: Yeah, absolutely. So, are there different types of injuries that can happen if patients don’t follow normal protocols? I mean, I know that we talked about manipulations to kind of get them there, so I assume that they’re fixable. And like what should a patient look for if they start to fall into one of these categories?
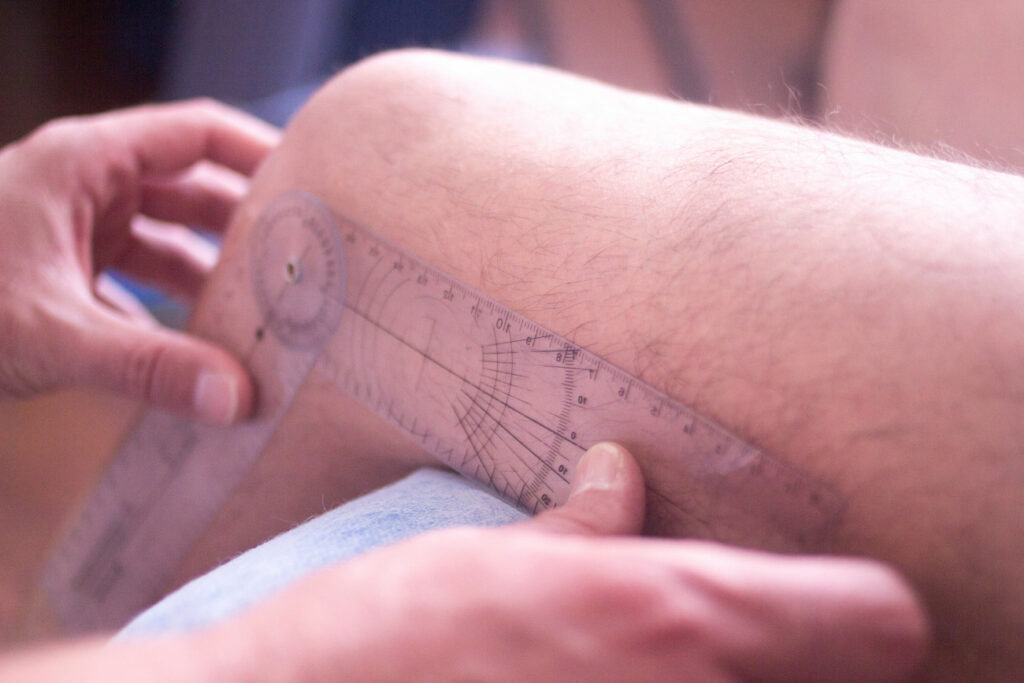
Dr. Knoll: Yeah. So, the big things are really just kind of – again, I mean, it’s what the mode, how the motion is doing, how the activity is doing. And even though there’s not a set like, okay, by four weeks, you should be here, eight weeks there, yeah, there are kind of some general principles. And so, if that motion isn’t getting where you’re all the way straight and getting past 90 or 100 degrees of flexion within about the first two weeks, that’s where you’re starting to kind of fall behind. So, that’s kind of where I get patients some parameters. I like you to be off assistance devices about that two to three-week mark, that kind of thing as well. So, there’s kind of some of those bigger kind of guiding principles that we kind of go with, and so we can use those to judge where people are at.
And they’re aware of where their goals are. I try and make sure that people are aware of where they need to be. I say, “Hey, of course, call me, let me know.” We’ll get them in, talk to figure out what’s going on.
But as far as the injuries and things like that, there can be injuries in there. Fortunately, we don’t run into really major injuries with them. Hardly ever met a person having infection and issues, the incision, things like that. But we being surgeons in general, I think, had a pretty good deal on that, but it’s pretty uncommon when we have one of those kinds of a major injury. Maybe aside if there’s an unfortunate fall or something like that, but the big injuries are pretty few and far in between. Most things are correctible.
Toree: Yeah, well, that’s good. So, don’t let a big surgery – folks that are watching – deter you from this. It’s a very rare instance that something will not turn out the way you want it to.
Dr. Knoll: Right, yeah.
Long-Term Maintenance of a Replaced Knee
Toree: Now, once a patient reaches full recovery, what is your typical advice to keep them from having to come back and see you again? So, any like long-term maintenance that’s associated with a knee replacement that they should know about?
Dr. Knoll: Yeah. So, based on what I said earlier, I bet you can guess what I’m going to say, but keep it strong. Keep it strong. Keep active. All our joints in our body and everything, they want to be moving.
One of the interesting things, and there’s not really a study out there, but I just at least seen this anecdotally is that when COVID hit, a lot of the population that used to go to the gym, or hey, I used to go walking and do this regularly, and that kind of came to a halt. So, I have a lot of people who when that hit, when that happened, over those ensuing months, and even six months afterwards, man, my knee hurts way more than ever now. These things are just hurting.
I think it’s like a car. If a car sits in the garage, and you don’t drive it, well, the battery kind of dies, and the oil gets thick, and all that. Your joints in your body meant to be moving, meant to be used. So, I see long term is using. And of course, that’s within reason. I mean, I don’t need you to go now and start a football career after having a replacement, but almost everything you can do. Go biking. Go hiking. Go swimming. Go on walks. Go golfing, bowling, whatever it is you want to, all those things. But staying active and keeping up with exercise. Keeping it strong and keeping that range of motion, that keeps you away from seeing me again. It really does.
Toree: Yeah. Well, a body in motion stays in motion, right?
Dr. Knoll: Absolutely, absolutely.
Dr. Knoll’s Patients on the PortableConnect
Toree: And I’ve got to talk about it since we’ve kind of brought it up at the beginning here. So, you’ve been using ROMTech’s PortableConnect for a lot of your patients’ rehabilitation treatment.
Dr. Knoll: Yeah.
Toree: What kinds of results and impact are you seeing with your patients so far since implementing that?
Dr. Knoll: I really love using it, and my patients have as well. So, I started using it in about April, so I’ve had it for about six or seven months now that I’ve been using it.
When I first found out about it, I kind of was like, huh, I like that, because it really goes along with kind of my philosophy, kind of the crawl-walk-run kind of thing, where the first thing is getting that motion. And right now, the traditional way of doing it is going to physical therapy two to three times a week, and that’s a session that a lot of patient dread, because you’re going there, and you have this therapist, very much means well, but they’re sitting here and kind of cranking on that knee and pushing it up. And you’ve got this one time every two or three days you’re doing that, and you’re trying to do exercises when you’re at home, but you don’t really know what you’re doing. Am I doing too much? Am I doing enough? And so, it becomes a real painful thing just to get that motion.
So, with the bike, being able to make those revolutions, and start out with that small arc of motion, having the passive mode that kind of transitions into the active mode, and doing it broken up five times a time, where these little sessions that you kind of do incrementally, it just makes it so much easier.
So, I’ve had patients, my favorite ones are the ones that I did a knee on say December last year, or before I had the bike do one side, and they go through traditional recovery, and do well with it. But then have had a second knee replacement now, and have the bike, and they say, “Man, I wish you had that the first time. It’s so much easier this time around.”
And I’ve had a number of people who, after finishing the bikes, say, “Man, I’m getting an exercise bike. Now, that I have this, I can get that motion, I want to kind of keep this going.” And obviously, that’s not the same thing if you just bought an exercise bike, but it’s an ongoing sort of thing that they see the value of it and everything.
So, it’s really been a good experience. I’ve seen patients come back getting off of assistance devices earlier. And the convenience, I mean, they really like. You don’t have to have, hey, who’s taking me to therapy, and sitting there for an hour twiddling their thumb while I do this three times a week. It frees them up. I’ve done where I don’t even send patients to physical therapy. They get their exercises and they work at home.
Toree: Wow, that’s awesome. And I mean, how long do they say? It takes about two or three weeks to create a new habit. So, if they’re on this PortableConnect and moving, all of a sudden, they have a habit to move. So, hopefully, yeah, it will keep them from seeing you again.
Dr. Knoll: Yeah.
Toree: All right, we’ve got just a couple more minutes left, so I wanted to ask one more question. What would you tell other orthopedic surgeons about the PortableConnect? For those that might be watching.
Dr. Knoll: So, I would say give it a chance. I mean, I would say that it’s always a little bit of a challenge of bringing something new in, because most of us that are doing knee replacements really get good results. Doing physical therapy works, and people do well, and in the end, they have a successful knee that they’re happy with. But I found that through the process, early weeks in recovery, it’s just more comfortable. People like it. They enjoy it, the convenience of it. Like I said, they’re doing it, breaking it up multiple times a day. Having a guided nature of doing it on a regular basis at home.
I’ve met patients who said, “Man, I wouldn’t do it another way.” I’ll do a wife, I’ve done their husband previously, and of course, they say, “Oh, this great.” And the husband was, “Where was that when I had mine?” So, I think it’s been a great addition. It’s easy to use. It actually, I think, makes even things easier for my staff, because there’s less questions, less issues that are happening, things like that. So, I’ll say give it a chance, because it’s really been a nice product.
Toree: Perfect. Well, thank you so much. I think that’s all I’ve got for you here today, Dr. Knoll. I appreciate you taking the time to answer some questions, and hang out with us.
Dr. Knoll: Happy to help. Thanks for having me.
Toree: Yeah, of course. So, for those of you that want to check out Dr. Knoll, you can visit him at www.tristate-ortho.com. They’re on Facebook. You can follow them on Instagram, @tristateorthopedics. And then of course, feel free to subscribe to our channel here, so that you can get all of this great information. Check us out at Romtech.com. And yeah, until next time.
Thanks again, Dr. Knoll. We appreciate it.
Dr. Knoll: Thanks for having me.
Toree: Yeah. See you guys later, bye-bye.
Disclaimer: The content discussed on this program is often medical in nature, and is used for informational purposes only. No content discussed should be taken as medical advice. Please consult your healthcare professional for any medical questions.
Privacy is also of the utmost importance to us. All people, places, and scenarios mentioned have been changed to protect patient confidentiality, unless given explicit written permission to share.
This podcast should not be used in any legal capacity whatsoever, including but not limited to establishing a “standard of care” in a legal sense, or as a basis for expert witness testimony.
View other news in: Rapid Recovery Report
